In early 2019, measles, a disease that had once been nearly universally eradicated reappeared in the United States, the Philippines and other regions. While frequent contact between individuals and communities through modern travel has made it easier for infectious diseases to spread. However, the measles epidemic has, at the time of writing, not yet had a major effect on China’s population. To some extent, this can be credited to the nation’s disease prevention and control system, which has come a long way since the nation’s founding. The government’s continued emphasis on vaccination and other disease prevention measures has also played an important role.
On April 9, 2019, amid the country’s worst measles epidemic in the past three decades, New York City Mayor, Bill de Blasio, declared a public health emergency that required residents living in parts of Brooklyn to be vaccinated or face fines of up to US$1,000. This was spurred by the figures released by the Center for Disease Control and Prevention on April 8, which showed a spike in the number of measles cases by 20 percent to 465 within the previous week – with most new cases originating from the borough of Brooklyn.
The United States was not alone: outbreaks also occurred in Europe, Japan and the Philippines. Also in 2019, Australia experienced a sharp rise in measles cases. Hong Kong, too, was affected, recording 62 new cases as of April 10, 2019. The cost of the vaccine within the region rose to a record high as many people simultaneously sought to get vaccinated. A female traveler from the Chinese mainland became Chinese mainland’s first confirmed measles patient after contracting the disease in Hong Kong, where her plane made a stopover en route to Guangzhou.
How did measles manage a resurgence when its vaccine has been readily available for decades? While frequent contact between individuals and communities through modern travel has made it easier for infectious diseases to spread, the epidemic has not gained the same hold among China’s vast population. To a large extent, this can be credited to the nation’s disease prevention and control system, which has come a long way since the nation’s founding, and the government’s continued emphasis on vaccination and other disease prevention measures.
The oldest recorded practice of inoculation is found in the text Douke Jinjing Fujijie (Collected Annotations on the Golden Mirror of Pox Diseases, 痘科金鏡賦集解) written by Yu Maokun (俞茂鯤) in 1727. According to this record, variolation (inoculation against smallpox) was first used in Taiping County (太平縣) Anhui Province during the reign of Emperor Longqing (隆慶) in the Ming dynasty (1567-72), making China one of the earliest known countries to practice inoculation. Nonetheless, throughout Chinese history, diseases like smallpox, measles and the plague still caused heavy casualties whenever they surfaced. The variolation method used in China, which used smallpox scabs from human patients as the inoculation agent, was later introduced into Europe and modified by using the less virulent cowpox to confer immunity. In 1805, the inoculation technique came full circle when cowpox was introduced to China. However, it failed to gain traction due to the high cost of the vaccine.
In 1919, China established the Central Epidemic Prevention Bureau (中央防疫處) a national vaccine and serum institute dedicated to public health and epidemic prevention, the first of its kind in Chinese history. Prior to its establishment, China had relied on imported vaccines. Yan Fuqing (顏福慶) Tang Feifan (湯飛凡) and other medical microbiologists who helped found the institute would play a key role in developing the nation’s public health sector and its vaccines.
Since its founding, the People’s Republic of China has regarded the research and development of vaccines and the vaccination of her people as matters of paramount importance. With limited resources to spend on health care it was recognized early on that it was cheaper to stop people becoming ill than having to treat their illness. In addition to the original Central Epidemic Prevention Bureau (renamed National Epidemic Prevention Bureau in 1925) and the Northwest Epidemic Prevention Bureau (西北防疫處) the new Ministry of Health (衞生部) established six major institutes to conduct research on biological products, one to serve each of the nation’s six major administrative regions (the Northeast, the North China, the Northwest, the Southwest, the South Central and the East China Administrative Region). The new institutes were tasked with preventing and controlling infectious diseases, as well as researching and developing vaccines. Thus began a new era in China’s vaccine industry.
The six institutes are: Changchun Institute of Biological Products (長春生物製品研究所), Beijing Institute of Biological Products (北京生物製品研究所), Lanzhou Institute of Biological Products (蘭州生物製品研究所), Chengdu Institute of Biological Products (成都生物製品研究所), Wuhan Institute of Biological Products (武漢生物製品研究所) and Shanghai Institute of Biological Products (上海生物製品研究所). Changchun Changsheng Bio-technology (長春長生公司), a company that had achieved notoriety following its vaccine safety scandal in recent years, had been founded on technology developed by the Changchun Institute of Biological Products.
Since the first National Health Congress (全國衛生會議) in 1950, the nation’s public health program had made disease prevention its priority. The same year saw the Ministry of Health announced the Temporary Regulations for Smallpox Vaccination (種痘暫行辦法) that launched China’s first nationwide scheme to provide free vaccinations for smallpox, Bacille Calmette-Guerin (BCG) and diphtheria-pertussis-tetanus (DPT) to all children. This was followed by a large-scale campaign to vaccinate the general populace.
The Temporary Regulations for Smallpox Vaccination ruled that all residents within the People’s Republic of China, regardless of nationality, must be vaccinated for smallpox according to the regulations; newborns must be vaccinated within six months after birth and revaccinated at the ages of 6, 12 and 18 years; revaccinations were required for those who had never been vaccinated for smallpox or had not received timely revaccinations; smallpox vaccination was free of charge for all individuals.
As the nation’s network of epidemic prevention institutions continued to grow and develop, a competent and professional brigade of vaccinators played a key role in eliminating infectious diseases, protecting public health and safeguarding the labor force’s productivity.
Meanwhile, academia also contributed to the effort by making numerous research discoveries: A team led by Tang Feifan (湯飛凡), for example, developed a live attenuated vaccine that helped bring the bubonic plague that ravaged Huabei (North China) region in 1950 under control. He also developed a technique that used ether to sterilize vaccines, enabling the mass production of high-quality smallpox vaccine under field-like conditions. This paved the way towards eliminating smallpox throughout the nation well ahead of schedule.
In 1961, smallpox became the first disease to be eradicated from China through the administration of vaccines. This achievement put China ahead of many countries, given that the World Health Organization only launched the global campaign to eradicate smallpox in 1959 and did not fulfill the goal until 1980.
The disease poliomyelitis, commonly known as polio, was once one of the greatest threat to children’s lives and well-being. In 1955, a polio epidemic erupted in the city of Nantong (南通) in Jiangsu Province, causing rapid and irreversible paralysis. Of the 1,680 people affected 466 died. The epidemic spread swiftly to various regions including Qingdao (青島) Shanghai (上海) Jining (濟寧) and Nanning (南寧). As polio broke out in numerous locations, widespread panic ensued. In 1957, Gu Fangzhou (顧方舟) a virologist who had recently returned to China from overseas, began conducting research on polio. In the following year, the Institute of Medical Biology of the Chinese Academy of Medical Sciences (中國醫學科學院醫學生物學研究所) a research facility dedicated to the research and development of the polio vaccine, was established in the countryside of Kunming (昆明).
In December 1960, the first batch of polio vaccine for 5 million people was successfully produced. It had an immediate effect in reducing disease incidence during the peak periods of various outbreaks. Gu Fangzhou’s team spent an additional year on researching and testing a form of vaccine that was both easy to transport and highly palatable to children. The resultant candy vaccine was a hit and would be remembered by several generations of Chinese people. For this, Gu Fangzhou was fondly known as Grandpa Candy.
In China, there is an old saying that “children are not truly out of Death’s clutches until they have had measles and smallpox.” According to the Ministry of Health’s statistics, back when the country had not yet launched its large-scale vaccination campaigns, the annual measles incidence in 1950-1965 was on average 590 cases per 100,000 people; in 1959, the annual number of reported cases skyrocketed to 10 million. Once the liquid vaccine for measles was administered, incidence of the disease gradually declined: by the mid-1970s, the average number of reported cases ranged from 1.5 million to 5 million per year.
There used to be a high prevalence of hepatitis B infection in China. In 1975, Tao Qimin (陶其敏) director of the Institute of Liver Diseases of Peking University Health Science Center (北京醫學院肝病研究所) successfully developed China’s first hepatitis B vaccine in near-field conditions. She then gave the technology and its production techniques - free of charge - to Changchun Institute of Biological Products.
In support of the World Health Organization’s Expanded Program on Immunization, China issued a Notice on Strengthening Planned Immunity (關於加強計劃免疫的通知) in 1978, and thus the country entered a new age.
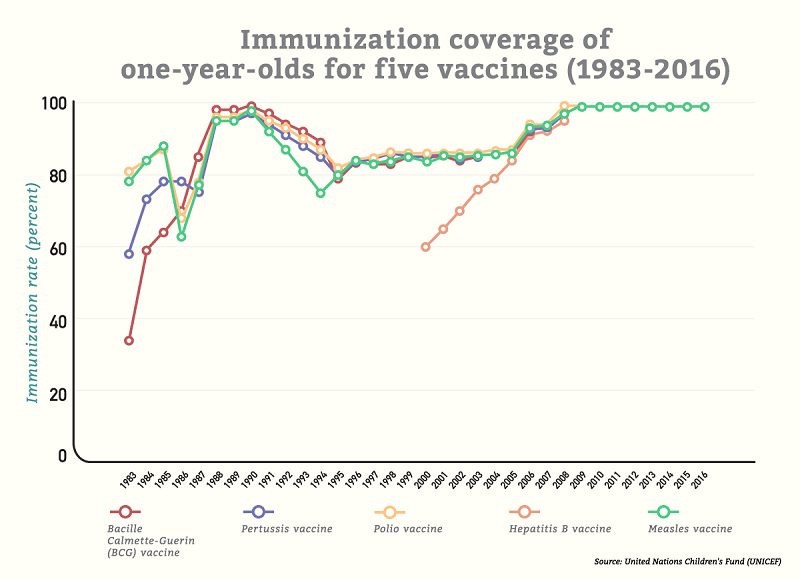
Since China started its universal immunization program for children the immunization rate among children has soared and the incidence and mortality from various diseases has decreased sharply. According to Ren Gaofu (任高福), director-general of the Chinese Center for Disease Control and Prevention (中國疾控中心), China currently maintains a nationwide immunization rate of 90 percent or higher through its planned immunity program.
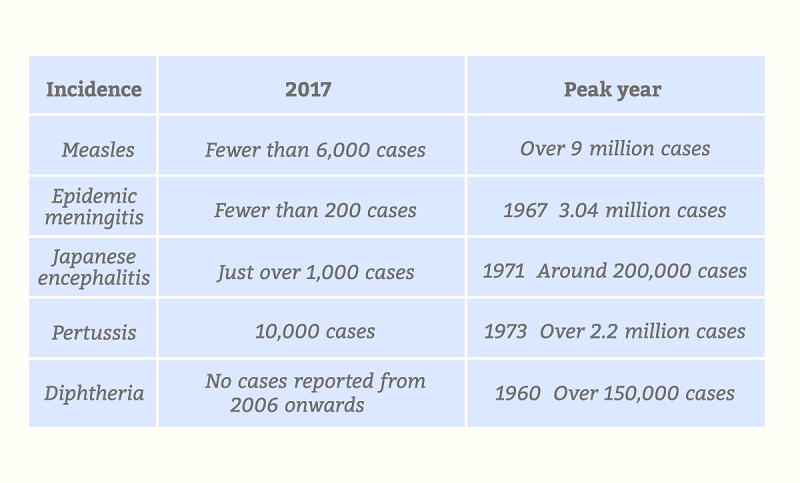
Vaccines have proven effective in controlling the spread of infectious diseases: In 2000, China fulfilled its goal of reducing the annual incidence of polio to zero; the incidence of Japanese encephalitis, measles, diphtheria, pertussis (whooping cough) and epidemic meningitis have also fallen to record lows.
The nation’s planned immunity program gradually expanded to provide coverage for more vaccines. In 2002, the program began to immunize newborns against hepatitis B; in 2007, a new acellular variety of the diphtheria-pertussis-tetanus (DPT) vaccine replaced the original version, and the hepatitis A vaccine, epidemic meningitis vaccine and measles-mumps-rubella vaccines were introduced into the national planned immunity program, boosting the total number of vaccines offered to 14 (for protection against 15 diseases).
Currently, vaccines in Chinese mainland can basically be divided into type 1 and type 2. Type 1 vaccines are provided by the government free of charge. Examples include the hepatitis B vaccine, the BCG vaccine and the live, attenuated oral vaccine for polio. Type 2 vaccines are non-mandatory and self-financed by citizens who choose to receive them. They are usually purchased, at market-determined prices, by the various inoculation organizations themselves. Type 2 vaccines include variations of type 1 vaccines such as the imported version of hepatitis B vaccine and the inactivated vaccine for Japanese encephalitis, as well as vaccines for diseases like chickenpox, influenza and rabies.
While the practice of vaccination becomes increasingly widespread, China’s work on vaccine research and development has also been making strides. It pioneered the development and use of a vaccine for the H1N1 strain of type A influenza and the development of the EV71 vaccine. This is currently the only vaccine that has proven effective in preventing severe Hand, Foot and Mouth disease. Other newly developed vaccines include a live, attenuated vaccine for hepatitis A, a vaccine for rotavirus infection, a hepatitis E vaccine and an avian flu vaccine for human use.
Nevertheless, as the medical sector undergoes marketization and deregulation and the vaccine industry becomes increasingly privatized, vaccine enterprises are gradually shifting focus from research and development to product sales. This trend is being driven by the industry’s unique characteristics - high technology, high investment, long cycle and high profit. While a high up-front investment is necessary, production costs at the later stage are low, so enterprises strive to recoup their investment as quickly as possible and maximize the profit margin through high volume sales.
This has led to the emergence of ineffective, counterfeit and unsafe vaccines that are a grave public health threat and can lead to other adverse social consequences. One of these is a rising public skepticism about the effectiveness and safety of vaccination. To make matters worse, speculation spread via the internet by an international movement against vaccination, fueled by unfounded fears of a relationship between vaccination and autism, has caused great distrust among parents many of whom now refuse to allow their children to be vaccinated.
To address these concerns, the State Council in 2019 established a system in which the State Administration for Market Regulation (市場監管總局) the National Health Commission (國家衞生健康委) and the State Food and Drug Administration (藥監局) are to lead joint inter-ministerial meetings on vaccine management, with the aim of reforming the country’s vaccine management system and tightening supervision across the whole production chain, from vaccine research and development to production, distribution and use.
China's historical experience with planned immunity programs is a testament to the importance of vaccination in safeguarding public health, raising life expectancy and supporting the international effort to eradicate infectious diseases. Without vaccines, China could not have succeeded in building a nationwide public health system from scratch. Today, vaccination is still internationally recognized as the most inexpensive, convenient and effective preventative measure against infectious disease. Vaccination will always be an integral part of any public health system. It is one of the most potent and economical weapons in any disease-fighting arsenal.
References:
A Historical Study of Disease Prevention and Control in the 1950s New China (20世紀50年代新中國傳染病防治工作的歷史考察) by Zhang Xiaoli (張曉麗) hprc.org.cn, Oct. 19, 2013
The Establishment and Development of China’s Planned Immunity Program - My Experience of Working for the Program (中國計劃免疫工作的建立與完善——我經歷的計劃免疫工作) by Zi Weikang (訾維康) Chinese Journal of Preventative Medicine (中華預防醫學雜誌) 2000 Issue 2
Chinese Society: System for Joint Inter-Ministerial Meetings to be Established for Vaccine Management and Regular Analysis of the Vaccine Safety Situation to be Conducted - The State Council (中國社會:建立疫苗管理部際聯席會議制度,定期分析疫苗安全形勢--國務院) Reuters, April 2, 2019
Measles Epidemic No Longer Contained in Europe and the United States as Japan, the Philippines and Various Countries Report Outbreaks (麻疹已超出歐美範疇,日本、菲律賓等多國疫情爆發) Q Daily (好奇心日報) Feb. 26, 2019
Residents of Brooklyn, New York to Receive Mandatory Vaccinations or Face Fine of HK$7,800 (紐約布魯克林強制居民接種疫苗 違者罰HK$7800) HK01.com, April 10, 2019
Hit “Like!” - A History of China’s Vaccine Development (中國疫苗發展史) Huzhou Center for Disease Control & Prevention (湖州市疾病預防控制中心) April 24, 2018
From Smallpox Variolation to Genetic Engineering: Snapshots of China’s Vaccine Development (從人痘接種到基因工程,中國疫苗發展剪影) Hongxing Xinwen (Red Star News) (紅星新聞) Aug. 1, 2018
40th Anniversary of Planned Immunity - Q&A (免疫規劃40週年問題答覆) National Health Commission (國家衞健委) July 13, 2018
An Atlas of Social Indicators of Children in China 2018, United Nations Children's Fund (UNICEF)